May 15, 2025
Most people think wisdom teeth only need attention when they start hurting. But when a wisdom tooth is growing sideways beneath the gums, serious damage can begin long before any pain appears.
Horizontally impacted wisdom teeth are one of the most destructive types of impactions. Many patients don’t realize there’s a problem until significant harm has already occurred.
Let’s take a closer look at why early evaluation matters.
Keep reading to find out what causes Burning Mouth Syndrome, when to seek treatment, and whether it can be cured.
Wisdom teeth, also called third molars, are the last teeth to develop, usually emerging between ages 17 and 25.
When there isn’t enough room in the jaw, these teeth can become impacted, meaning they’re trapped beneath the gums and bone. In a horizontal impaction, the tooth lies sideways and pushes directly into the roots of the neighboring second molar.
Instead of erupting upright like normal teeth, it presses forward, creating constant pressure against a healthy tooth you rely on every day.
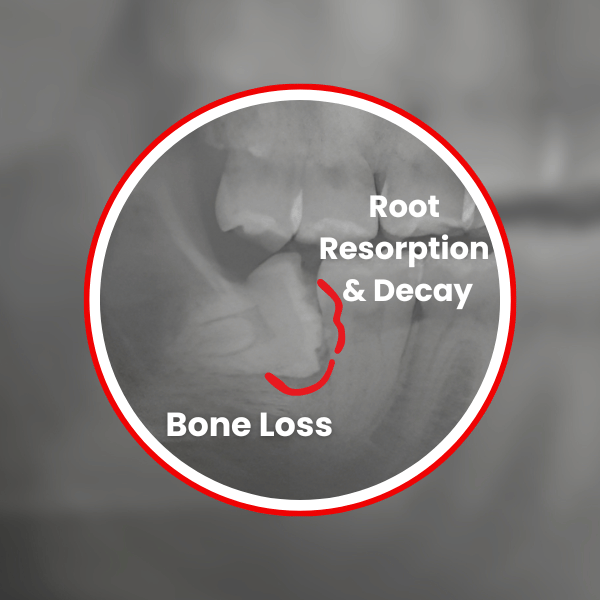
Horizontally impacted wisdom teeth rarely stay harmless beneath the surface. Over time, the pressure against the adjacent molar can cause:
By the time symptoms such as pain, swelling, or a visible cavity appear, the damage may already be extensive. In some cases, both the wisdom tooth and the damaged second molar must be removed.
Horizontally impacted wisdom teeth often cause subtle symptoms at first. You might notice:
Bad breath or a persistent, unpleasant taste can signal bacteria collecting around a partially impacted tooth. In more advanced situations, facial swelling, difficulty opening your mouth fully, or throbbing pain radiating toward the ear or jaw may develop.
Because early signs can be easy to overlook, routine dental X-rays are essential. Impacted wisdom teeth are often discovered on imaging before they cause noticeable symptoms. Detecting the problem early allows for simpler treatment and helps protect the healthy teeth you depend on every day.

Horizontally impacted wisdom teeth are often hidden beneath the gums and bone, making them impossible to evaluate without dental imaging.
A panoramic X-ray allows your dentist to see the exact angle and position of the wisdom tooth, determine whether it is pressing against the neighboring second molar, and identify early signs of bone loss or root damage. If the roots appear close to the inferior alveolar nerve, a 3D cone beam CT scan may be recommended to assess the area more precisely and plan safe removal.
When removed at the appropriate time, horizontally impacted wisdom teeth can usually be treated with a controlled, predictable procedure. The area is numbed with anesthesia, and sedation may be used to keep you comfortable. In some cases, the tooth is divided into smaller pieces so it can be removed more easily and with less pressure on the surrounding bone.
Mild swelling and soreness are common for a few days and can usually be managed with medication, cold compresses, and rest. Most patients return to normal activities within a few days.
Removing the tooth at the right time typically allows for faster healing and a smoother recovery than waiting until more serious problems develop.
The late teens and early 20s are often the best time to evaluate and, if needed, remove wisdom teeth. During this stage:
Addressing the issue early helps protect your main chewing teeth and lowers the chance of needing more complex treatment later.
If removal is delayed, the roots may grow closer to the inferior alveolar nerve in the lower jaw. Surgery at that stage can carry a higher risk of temporary and, in rare cases, permanent numbness or tingling in the lips, chin, or tongue.
If you’re in your 20s and haven’t had your wisdom teeth evaluated, now is a good time to schedule a check. The absence of pain doesn’t always mean everything is healthy.
At All Smiles Dentistry, we use digital imaging and a thorough clinical evaluation to determine whether your wisdom teeth are developing safely or if early removal could prevent future complications.
Protect your smile by acting early. A simple visit today could help you avoid pain, complex treatment, and damage to the teeth you rely on most.
Symptoms can include pain as well as swelling, jaw stiffness, or difficulty opening your mouth. Some impacted teeth show no symptoms; that’s why regular checkups are important.
Not always. Even without pain, they can damage neighboring teeth, bone, or gums over time.
Yes. Removing them in your late teens or early 20s usually results in easier surgery, faster recovery, and fewer risks of complications like nerve damage or tooth decay.
The answer is yes. Horizontally impacted teeth can push against second molars, which can cause decay, bone loss, or even root damage.
Most people feel better within a few days, but full healing of the gums and bone may take a few weeks. Your dentist will guide you on proper care.
Not always. If they’re properly aligned, fully erupted, and easy to clean, they may not need removal. Your dentist can determine what’s best for you.

Do You Need a Bone Graft Before Getting Dental Implants?
Root Canal Treatment: How It Saves Natural Teeth and Prevents Infection


Stop Waiting for Pain: Why Prevention Beats Costly Dental Treatments

Pulpotomy vs. Pulpectomy: What’s the Difference
| M | T | W | T | F | S | S |
|---|---|---|---|---|---|---|
| 1 | 2 | 3 | ||||
| 4 | 5 | 6 | 7 | 8 | 9 | 10 |
| 11 | 12 | 13 | 14 | 15 | 16 | 17 |
| 18 | 19 | 20 | 21 | 22 | 23 | 24 |
| 25 | 26 | 27 | 28 | 29 | 30 | 31 |
